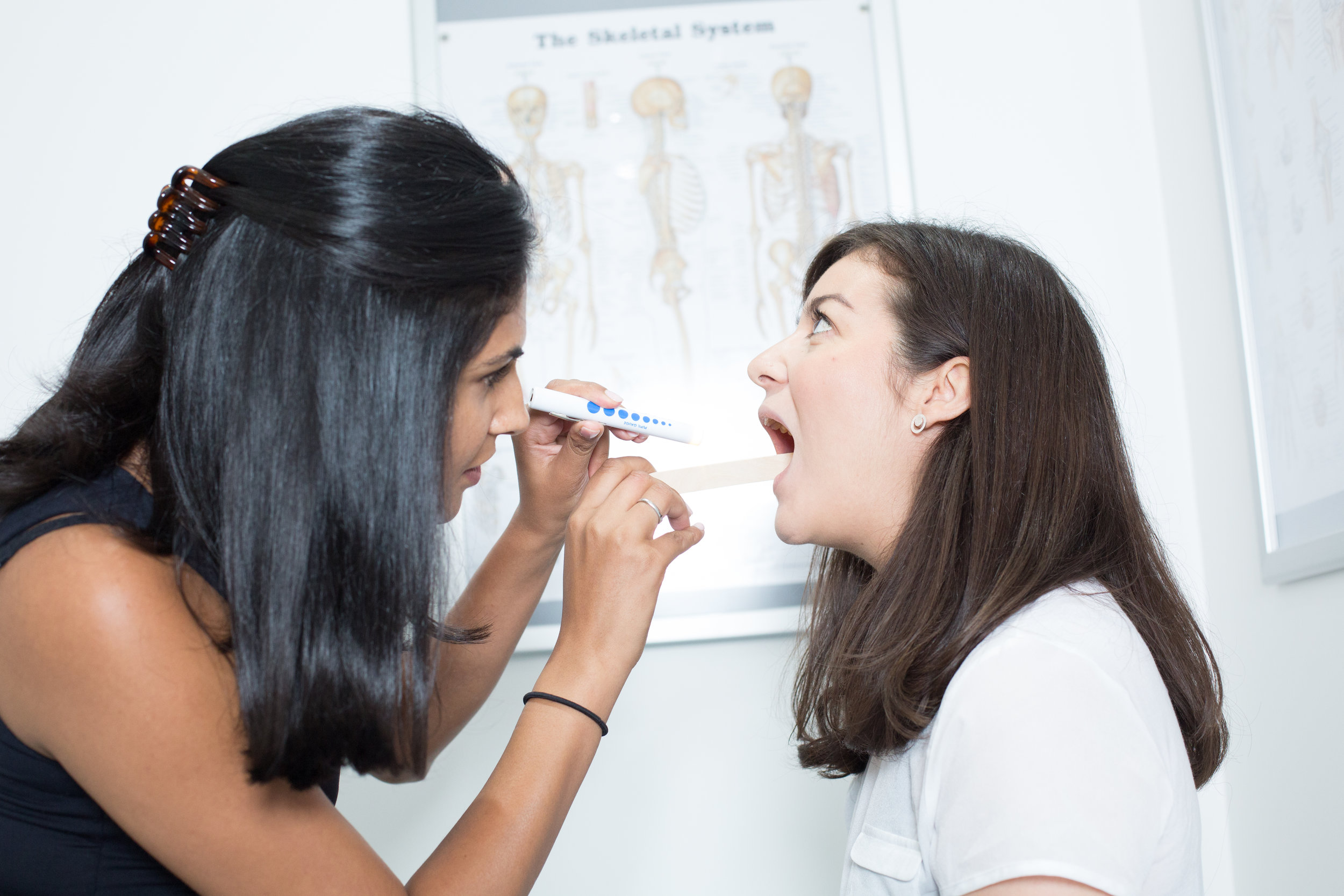
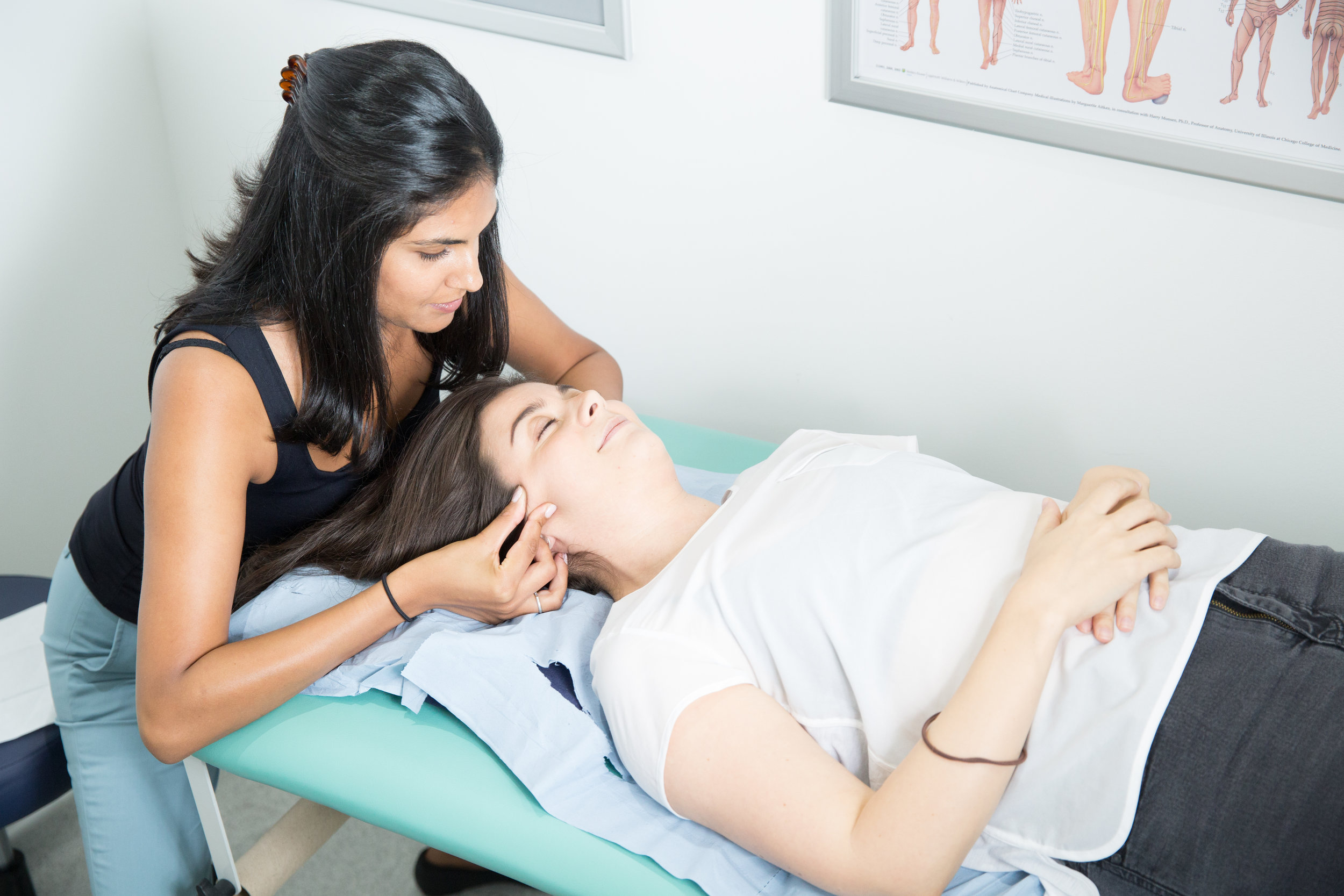
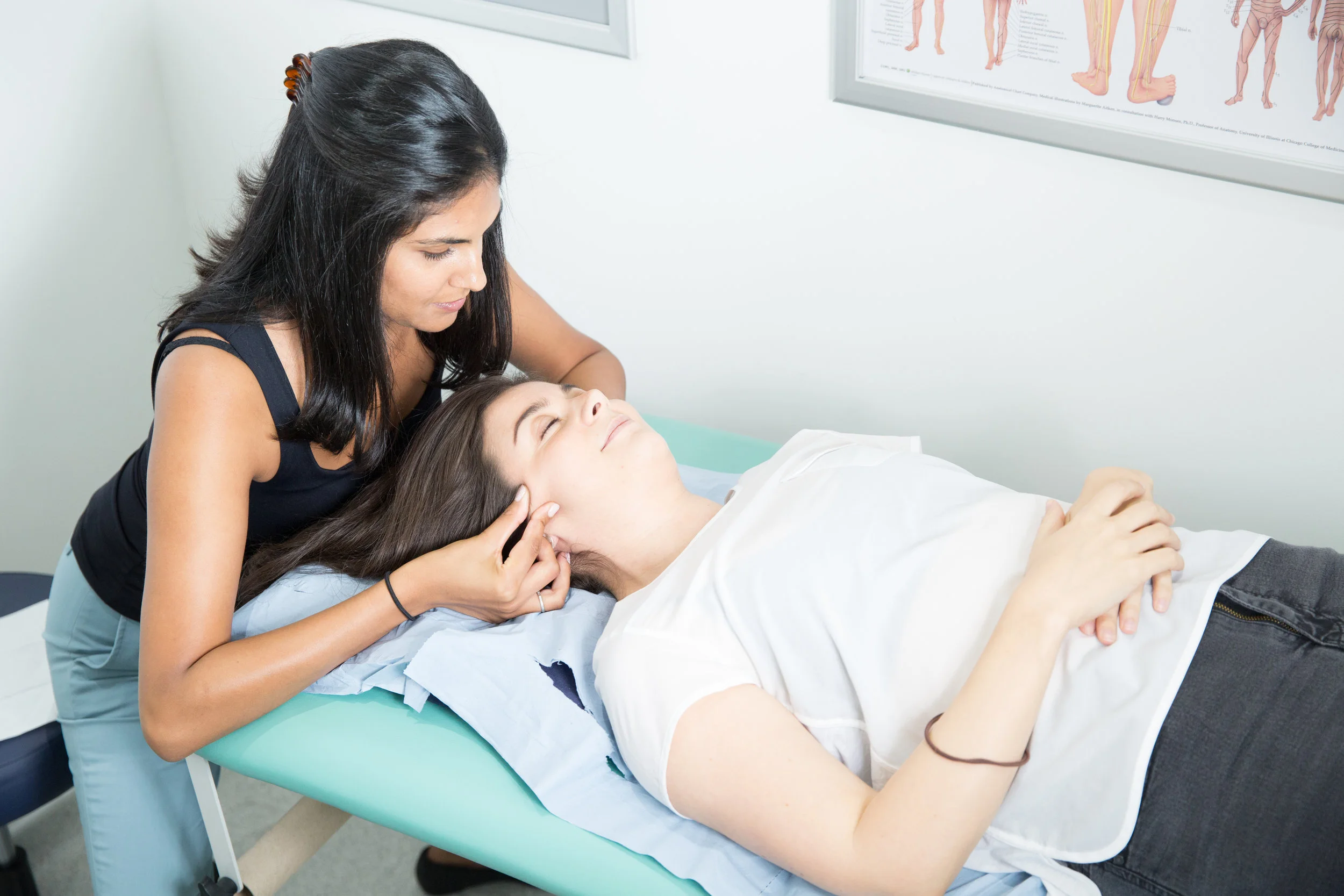
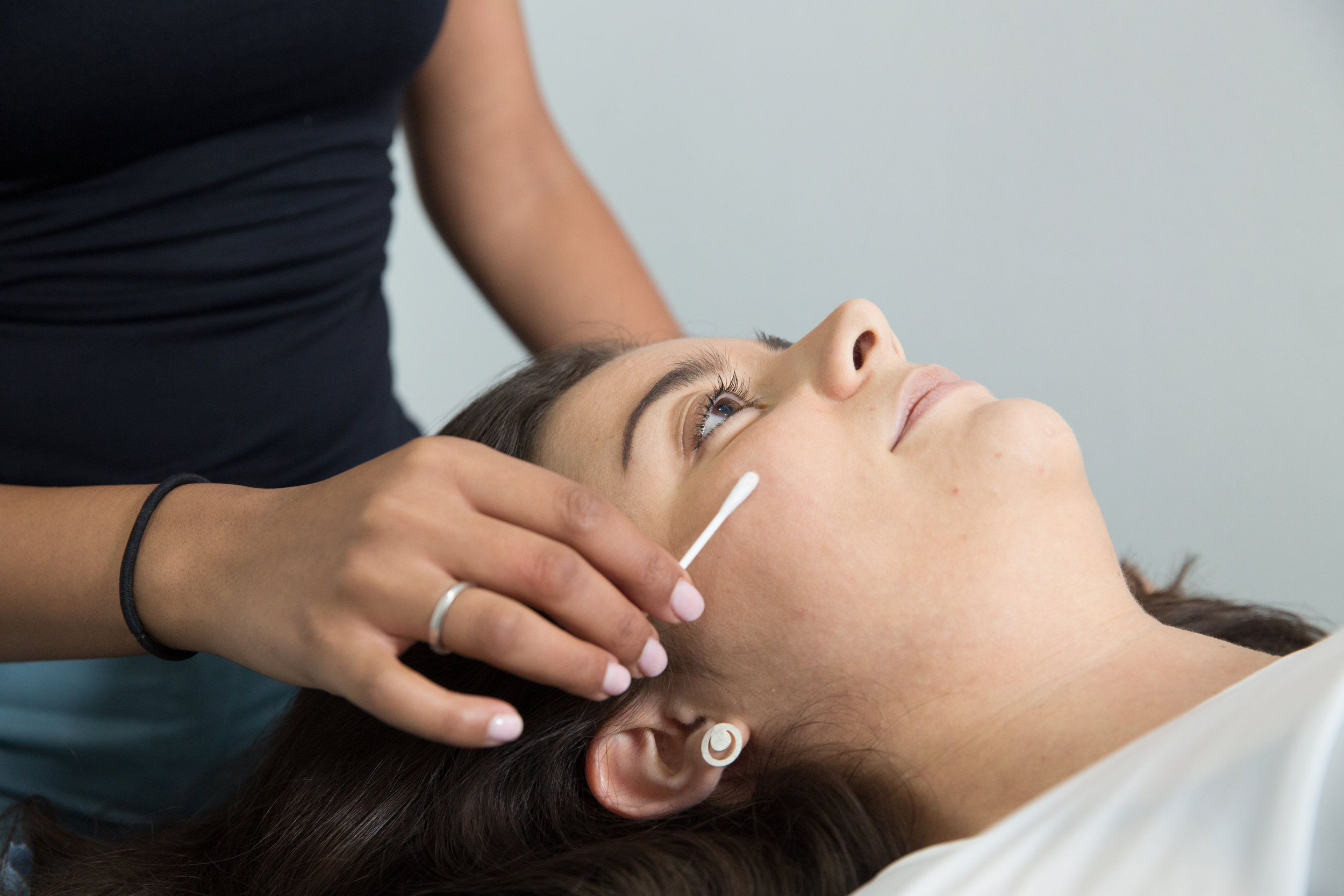
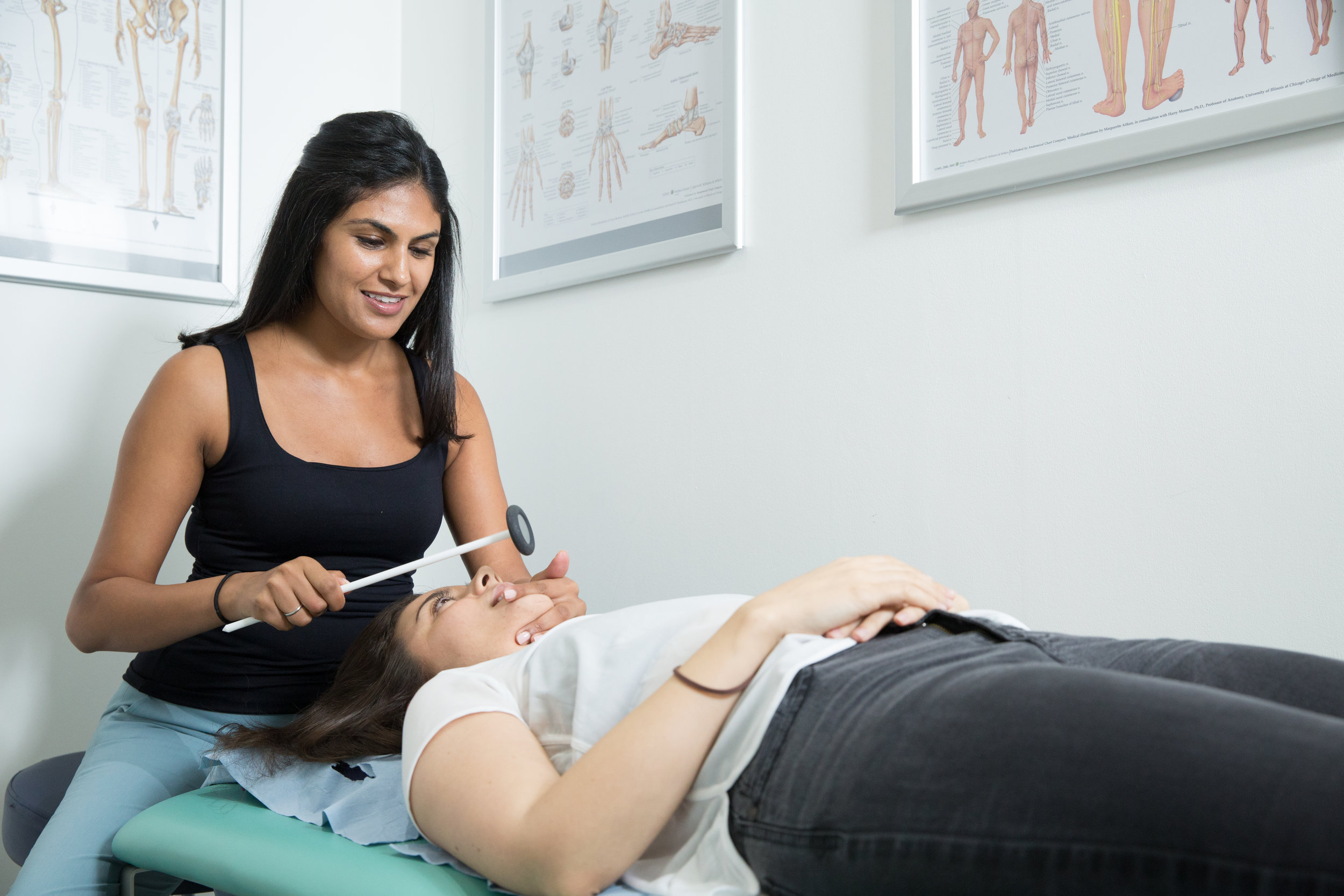
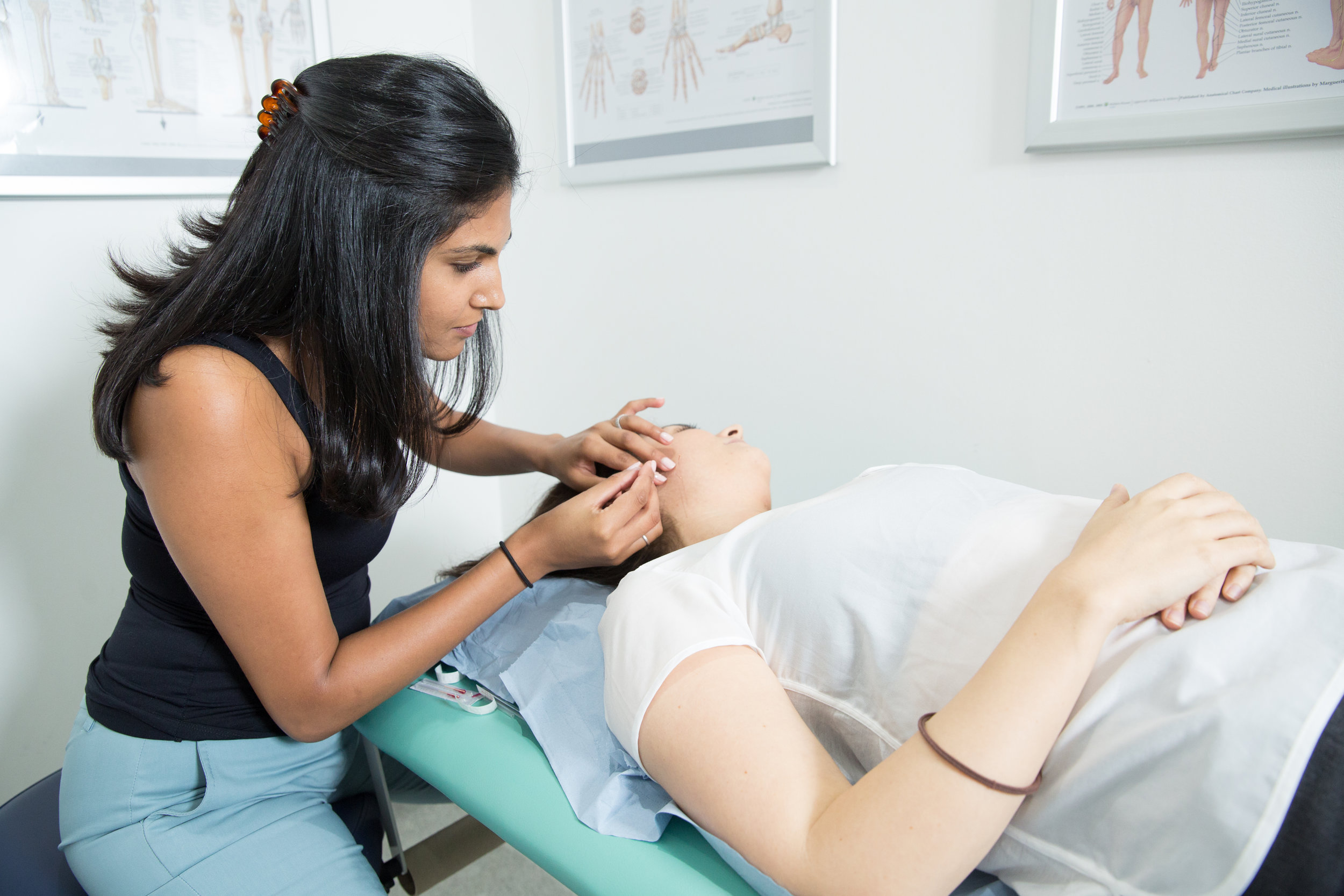
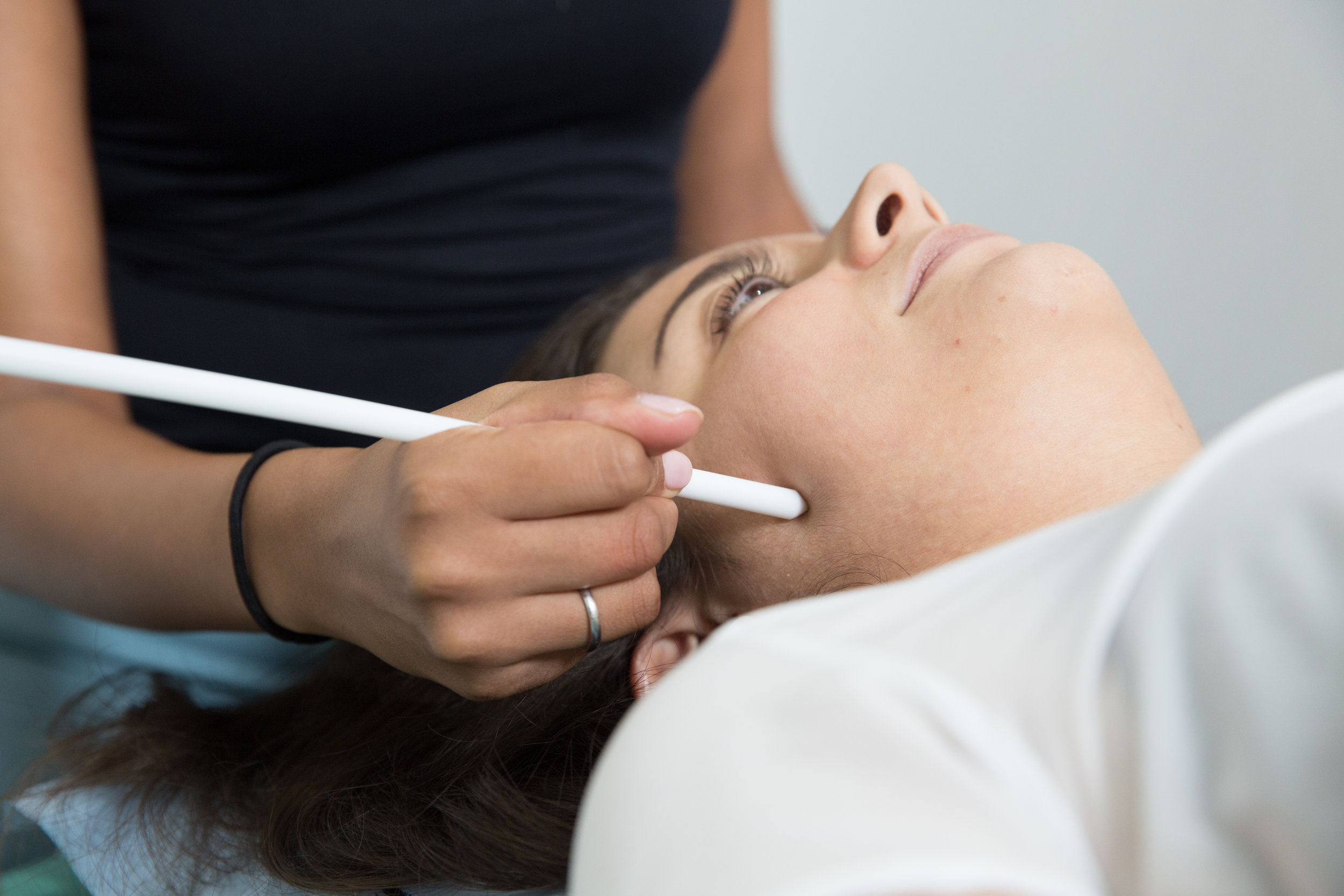
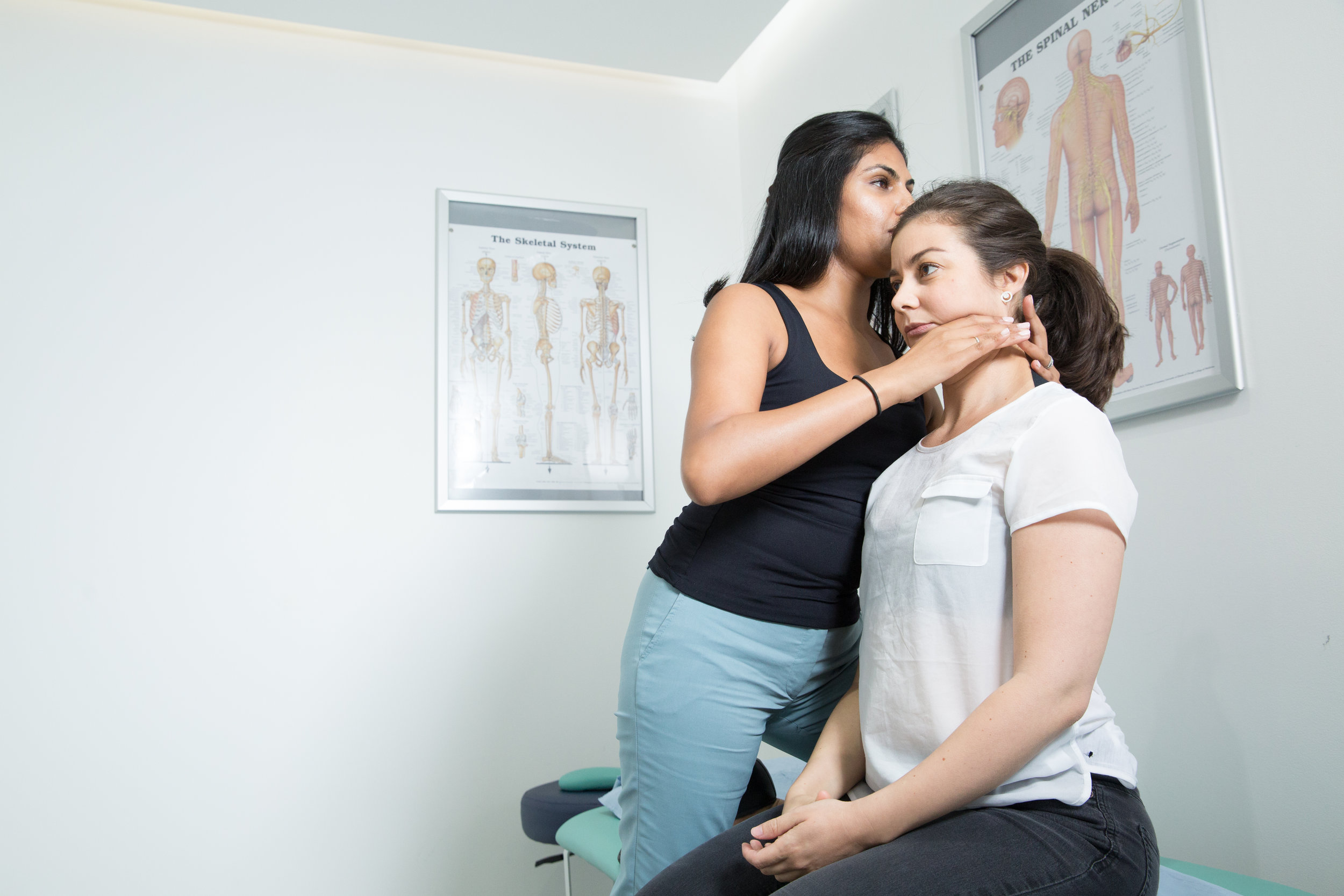
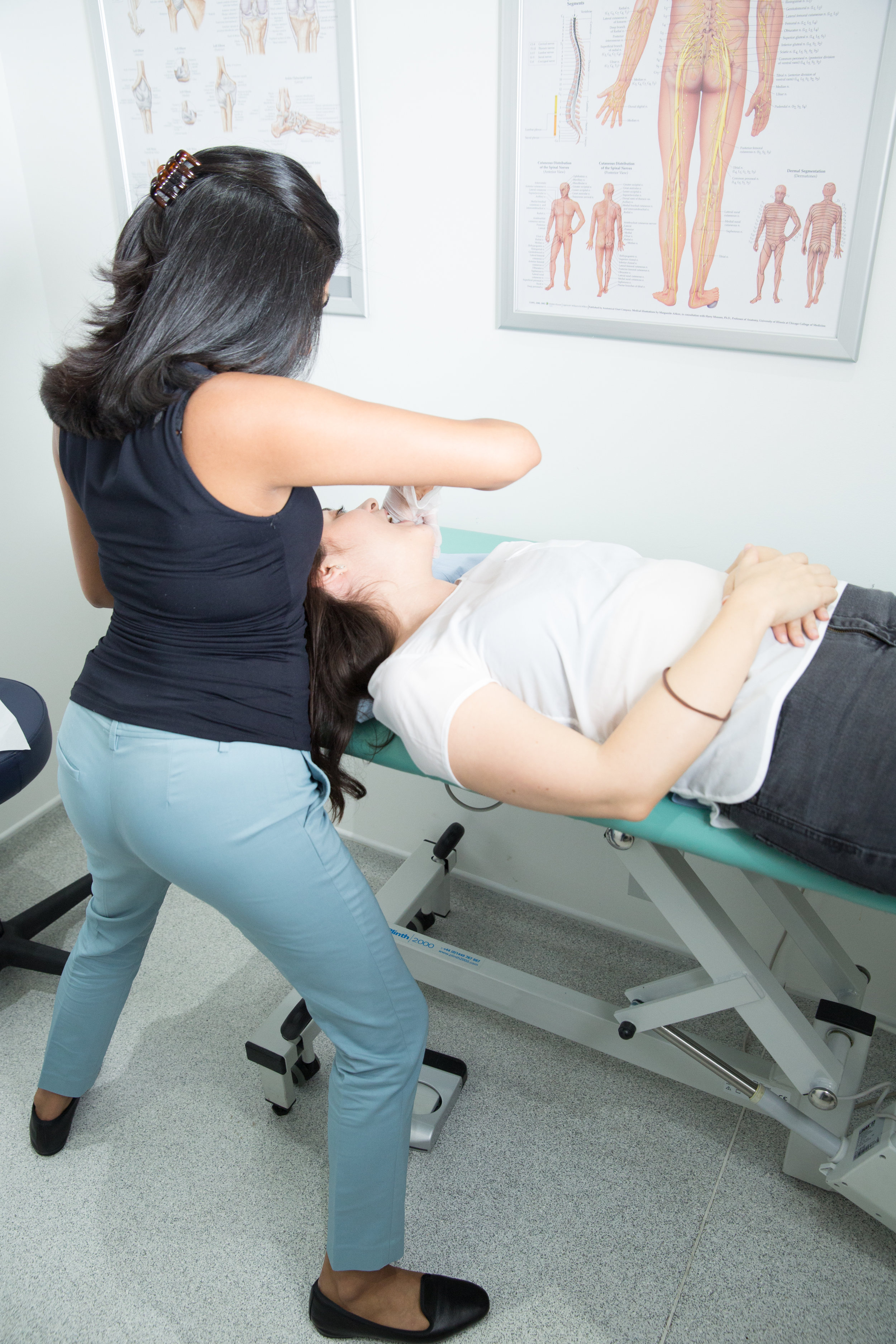
TMJ Dysfunction
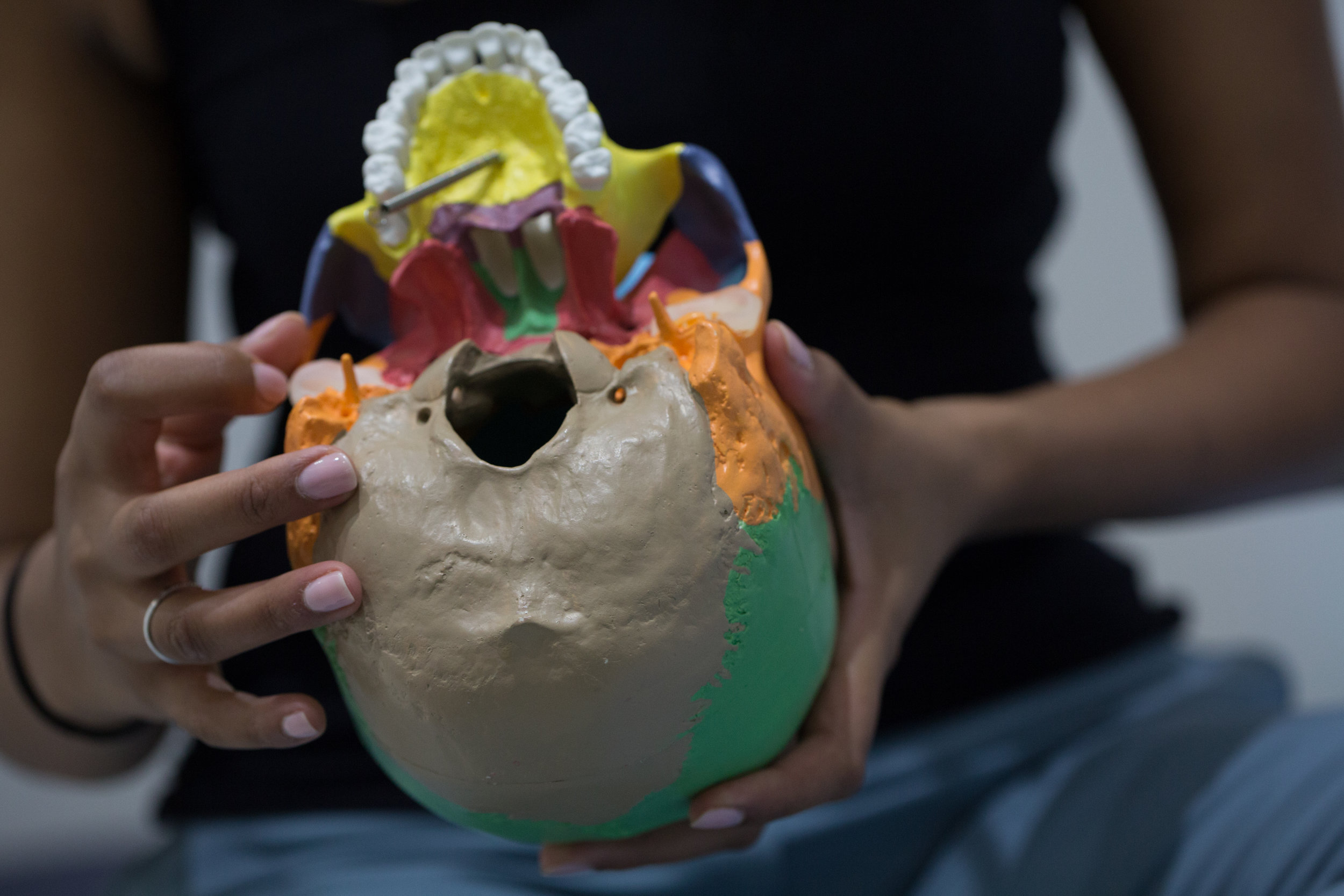
The Temperomandibular Joint (TMJ) is one of the most commonly used joints in the body and it also happens to be the most complicated. The TMJ and its associated muscles are commonly implicated in facial pain and headaches. The TMJ is formed between the skull and the jaw bone (mandible). Between the joint there is an intra-articular disc that is attached to the muscle and the back attached to the skull via retrodiscal tissues. The muscles associated with the TMJ are also know as the muscles of mastication. They move the jaw for chewing and speaking. The left and right TMJ muscles must work together as any malalignment can cause pain.
Bruxism
Muscular pain is the most common complaint which is a result of muscle imbalance or overuse due to bruxism. Bruxism is excessive clenching or grinding of the teeth that is not part of the normal chewing or talking movements of the jaw. Most patients have no idea they clench or grind as much as they do especially if it happens overnight while they sleep. Bruxism overworks the facial musculature which leads to pain as the muscles fatigue.
Discogenic Pain
The disc can sublux (dislocate) out of its normal positon. Uusally the disc moves too far forward and restricts the mouth from opening. This can occur as a result of an acute trauma or prolonged bruxing. During teeth clenching there is tension on the retrodiscal tissues which eventually overstretch as time goes on. There are 3 stages of disc subluxing:
Subluxing with relocation of the disc on the mouth opening
Subluxing without reloaction of the disc on opening without disc damage
Subluxing with relocation of the disc on opening with disc damage.
Other causes: Less commonly the joint structures can be affected with rheumatoid arthritis or infection.
Symptoms
facial pain
pain in or around the jaw joint or ear
being unable to open the mouth comfortably
clicking, popping, grating sounds of the jaw joint
headaches
the bite feeling uncomfortable
swelling on the side of the face
neck, shoulder and back pain
tinnitus
pins and needles or numbness in the face
migraines
anxiety
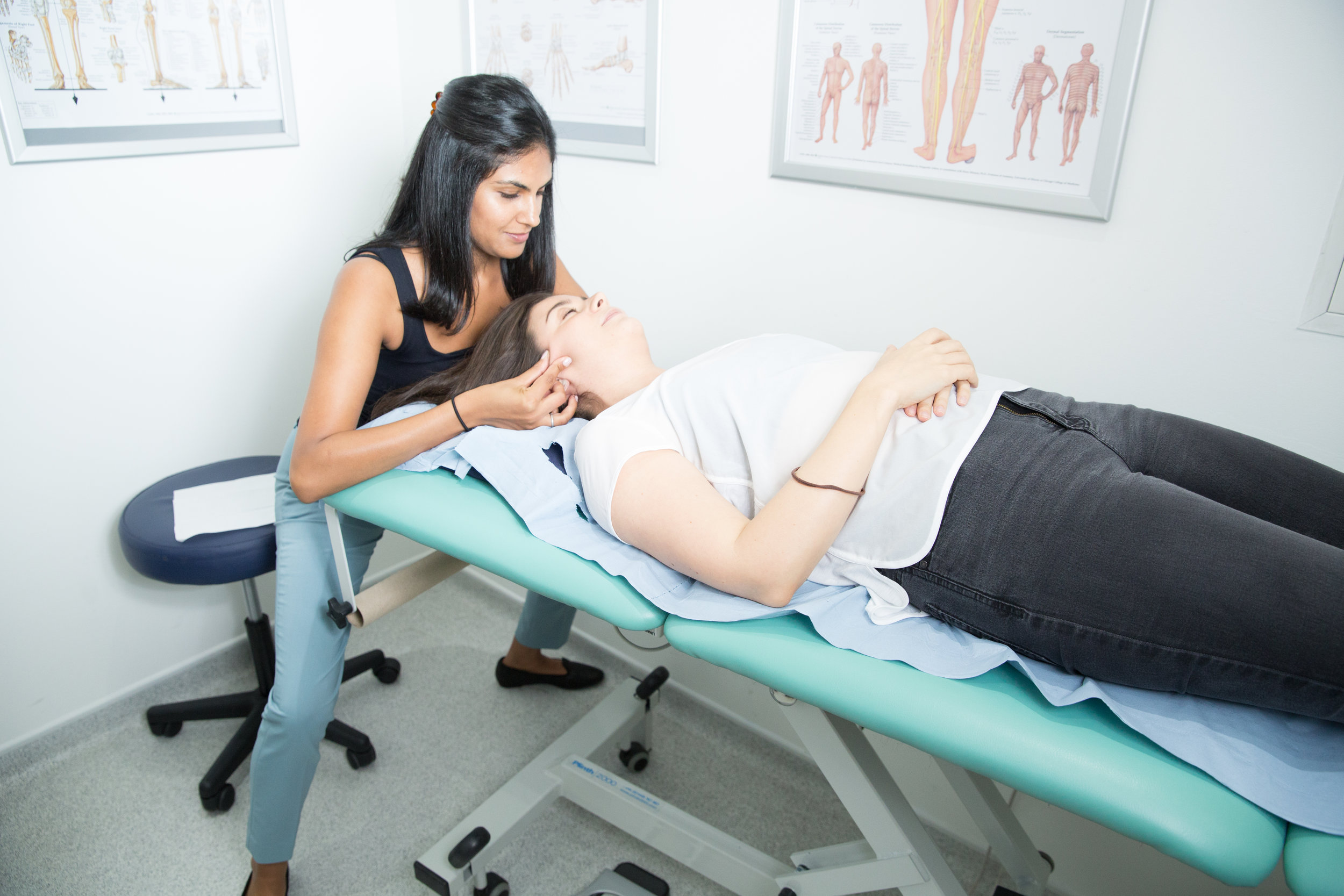
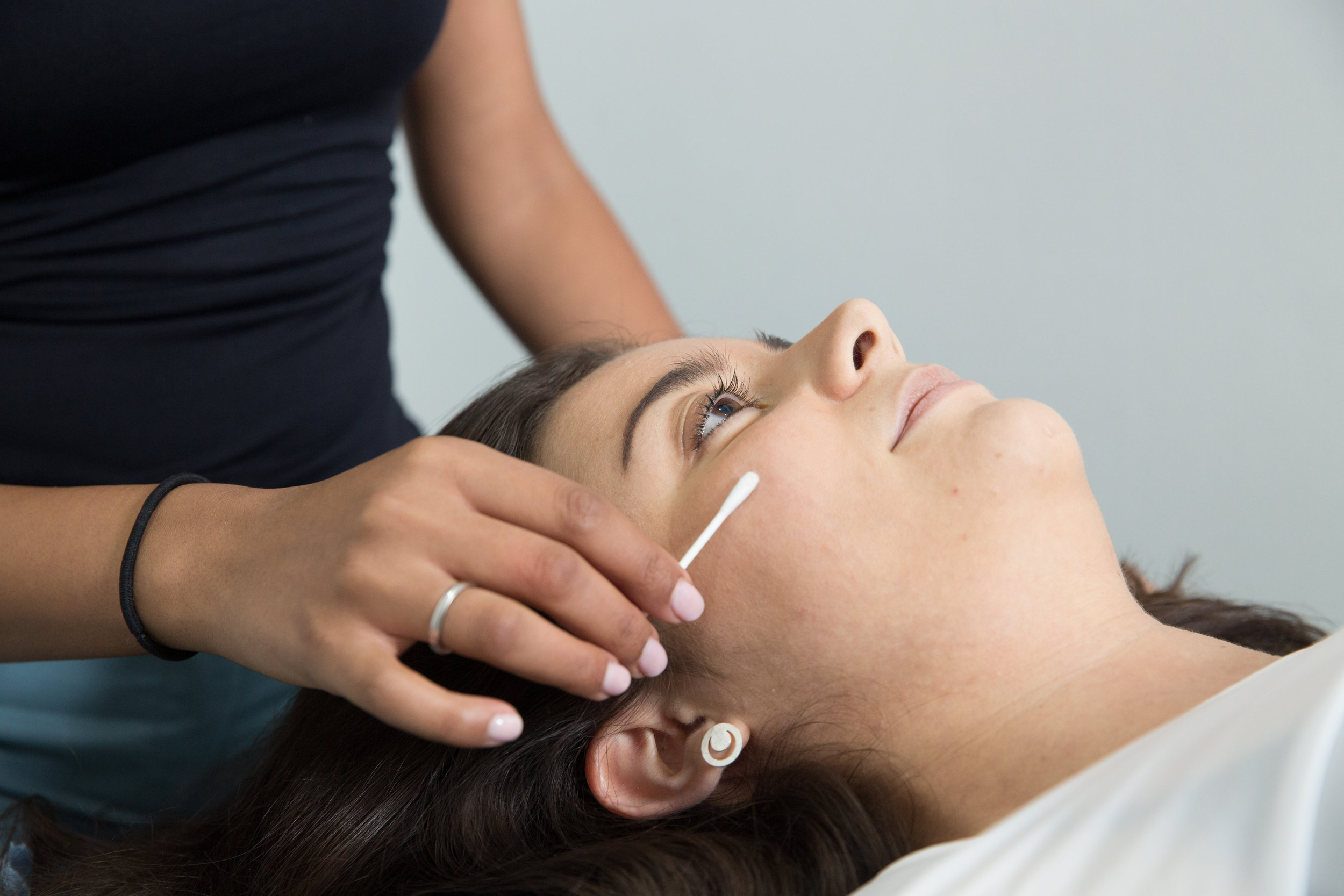
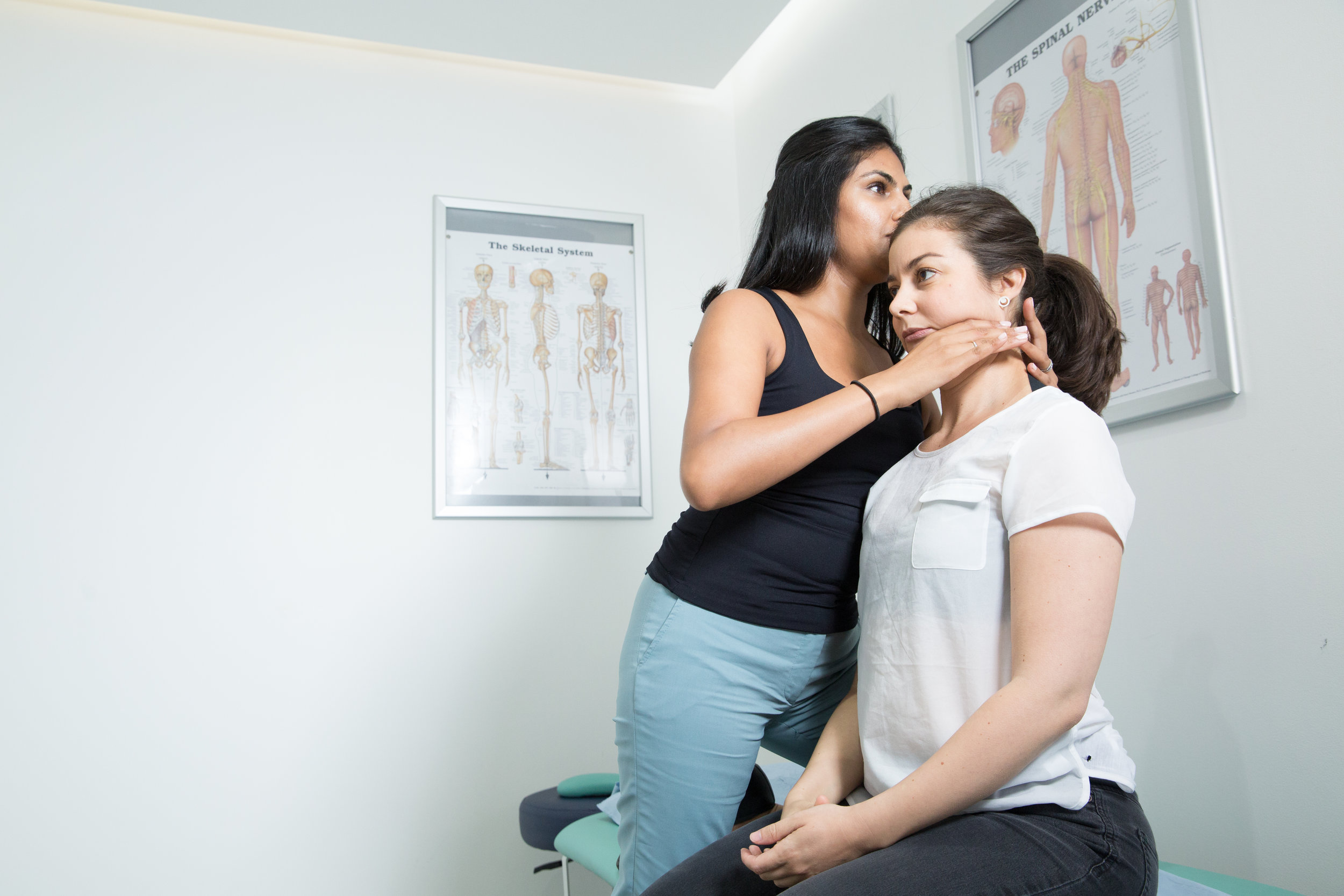
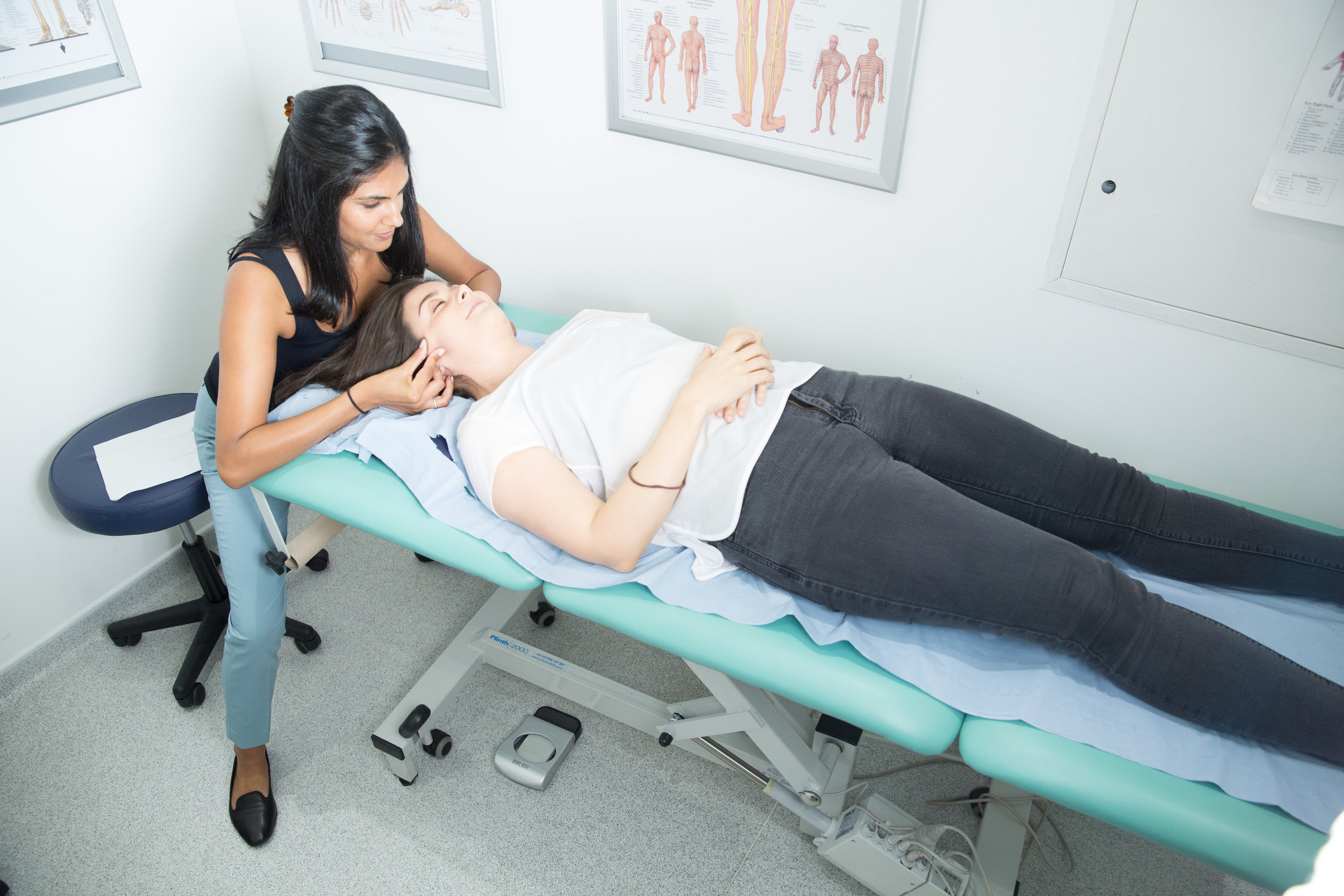
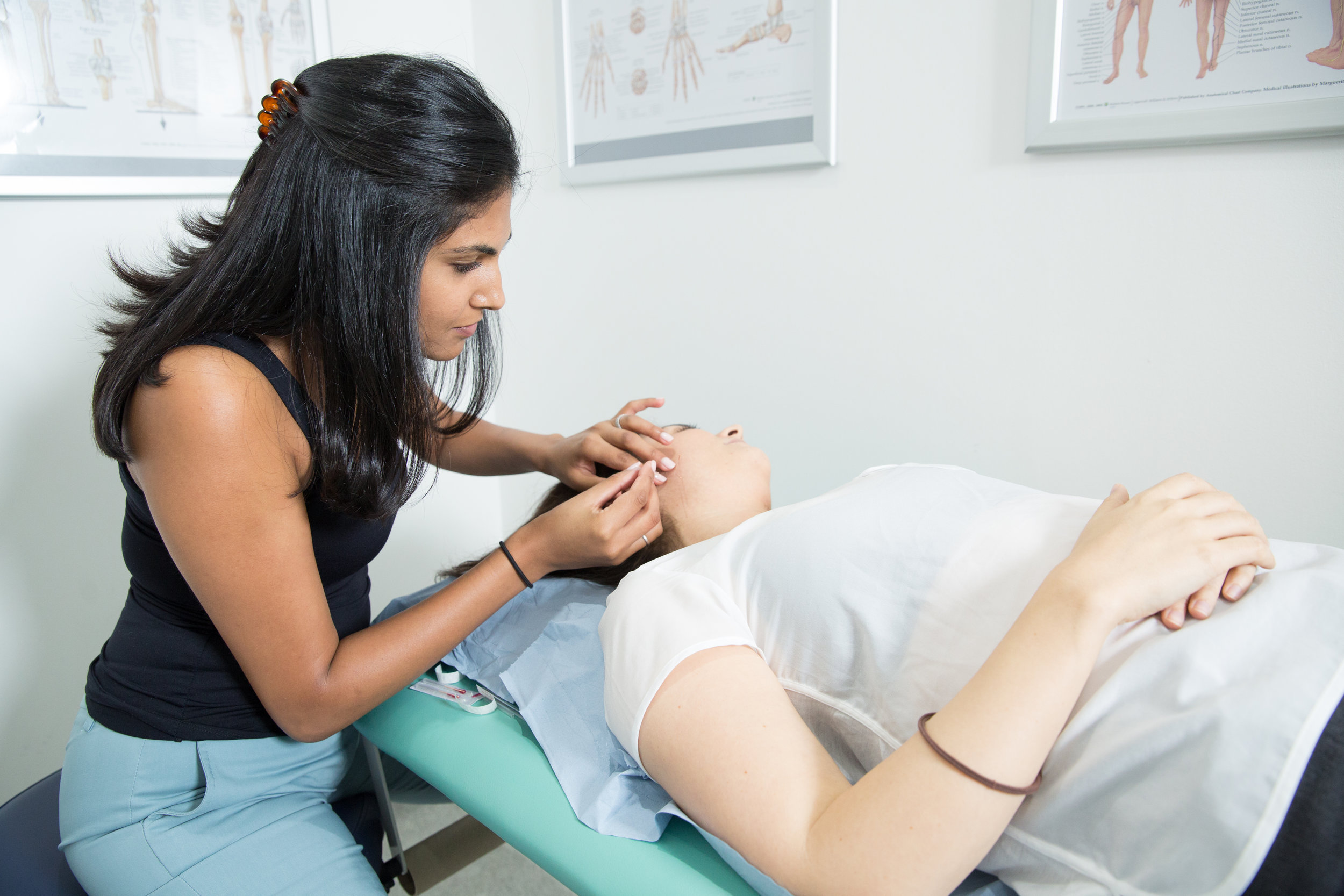
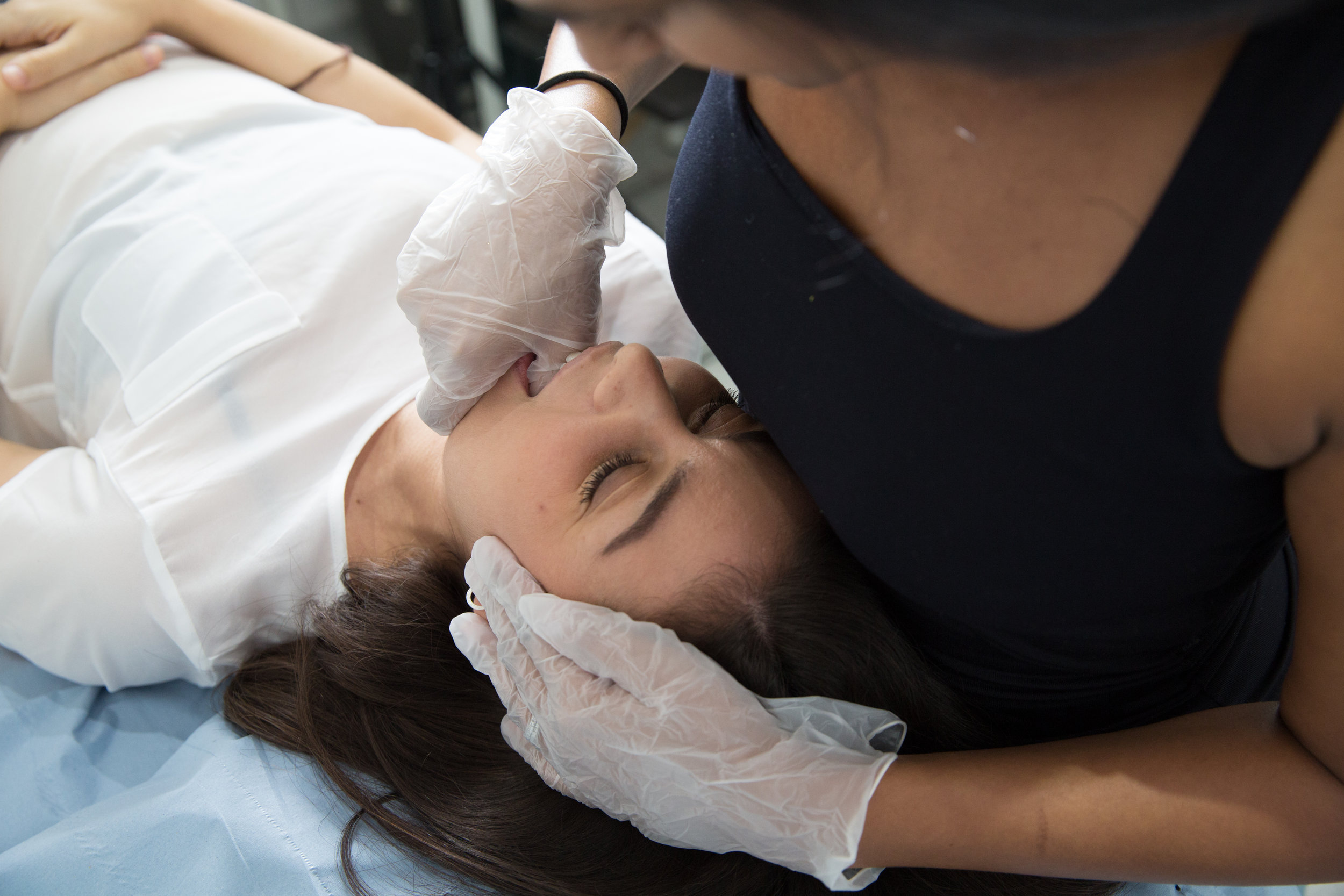
How I Treat TMJD
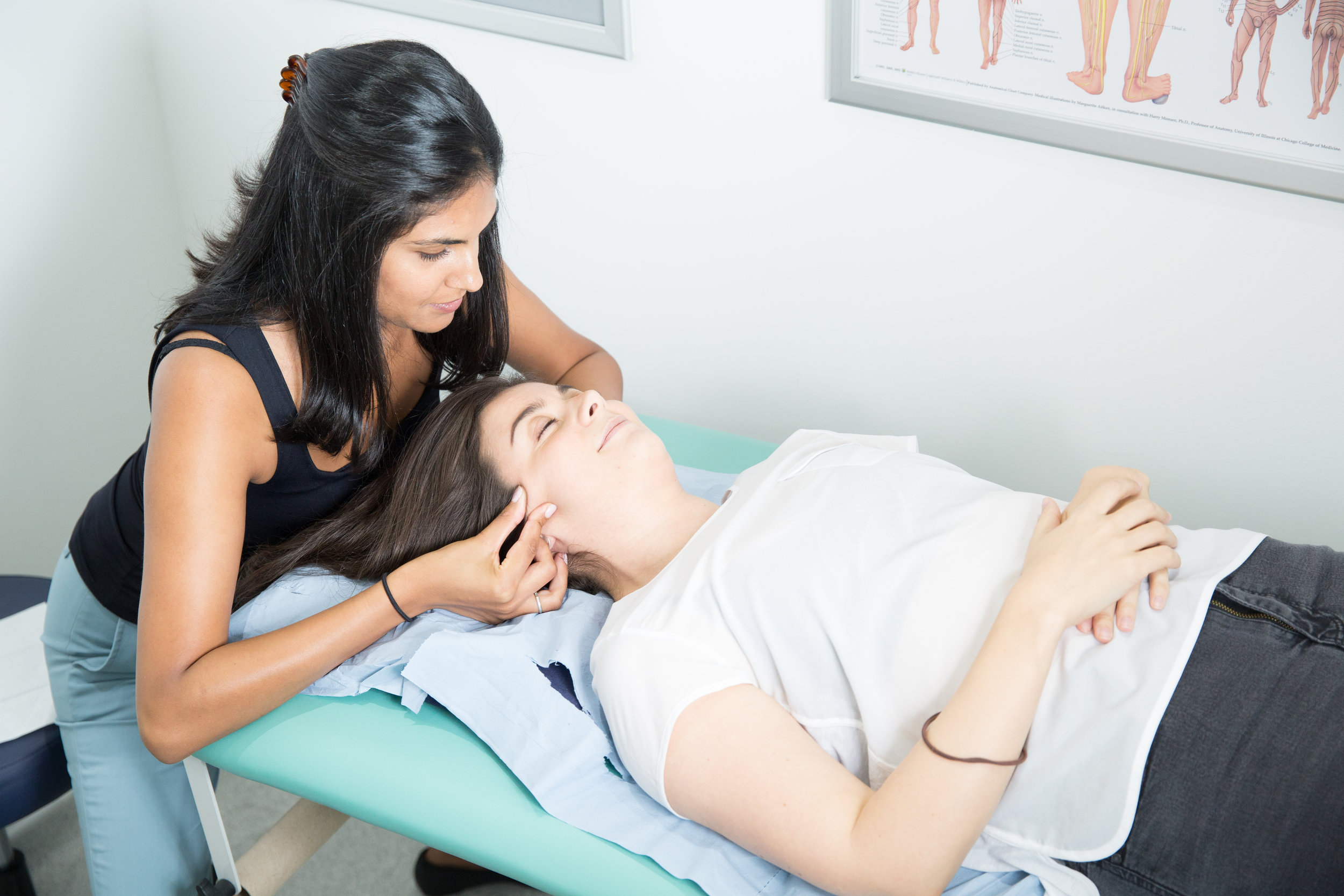
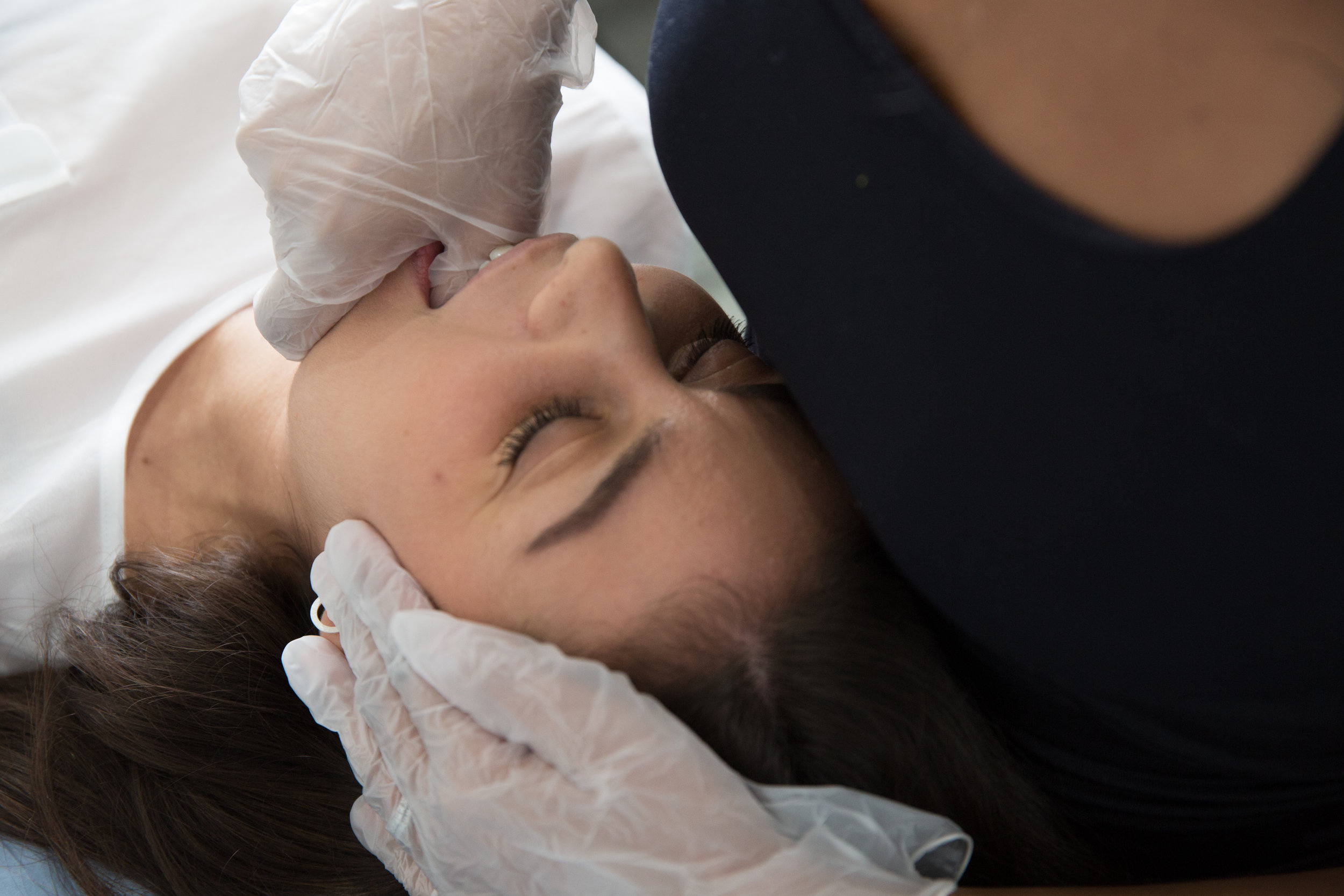
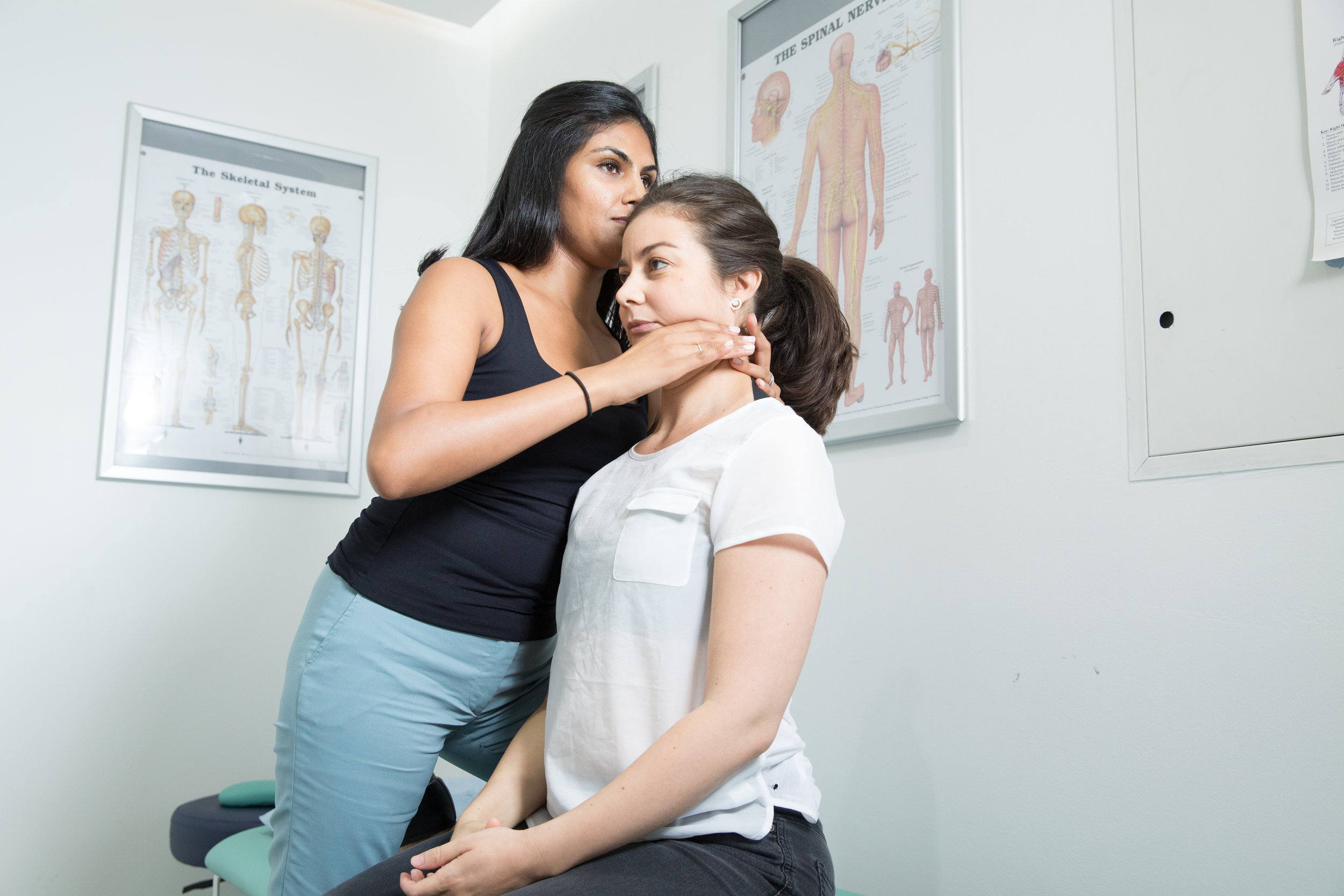
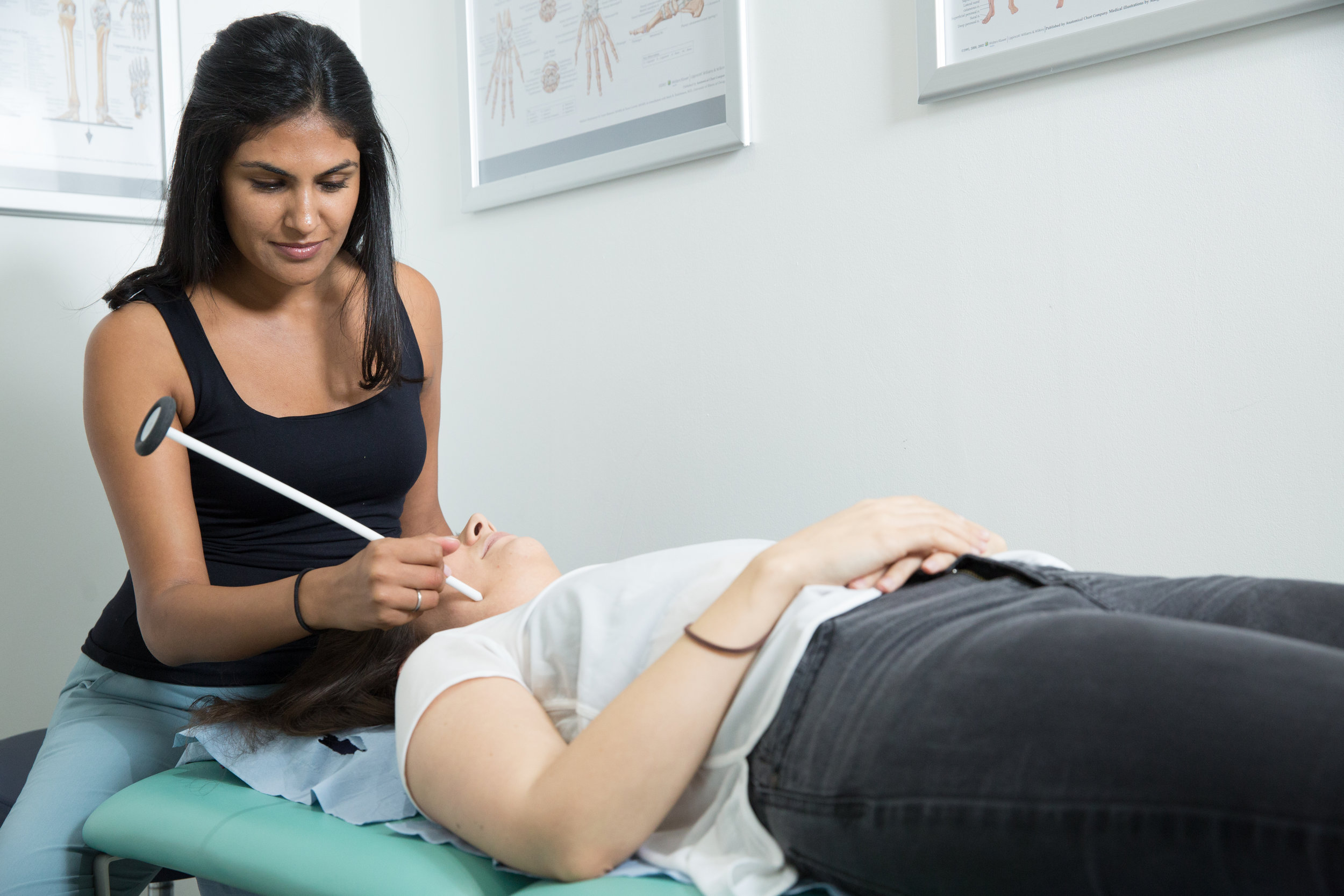
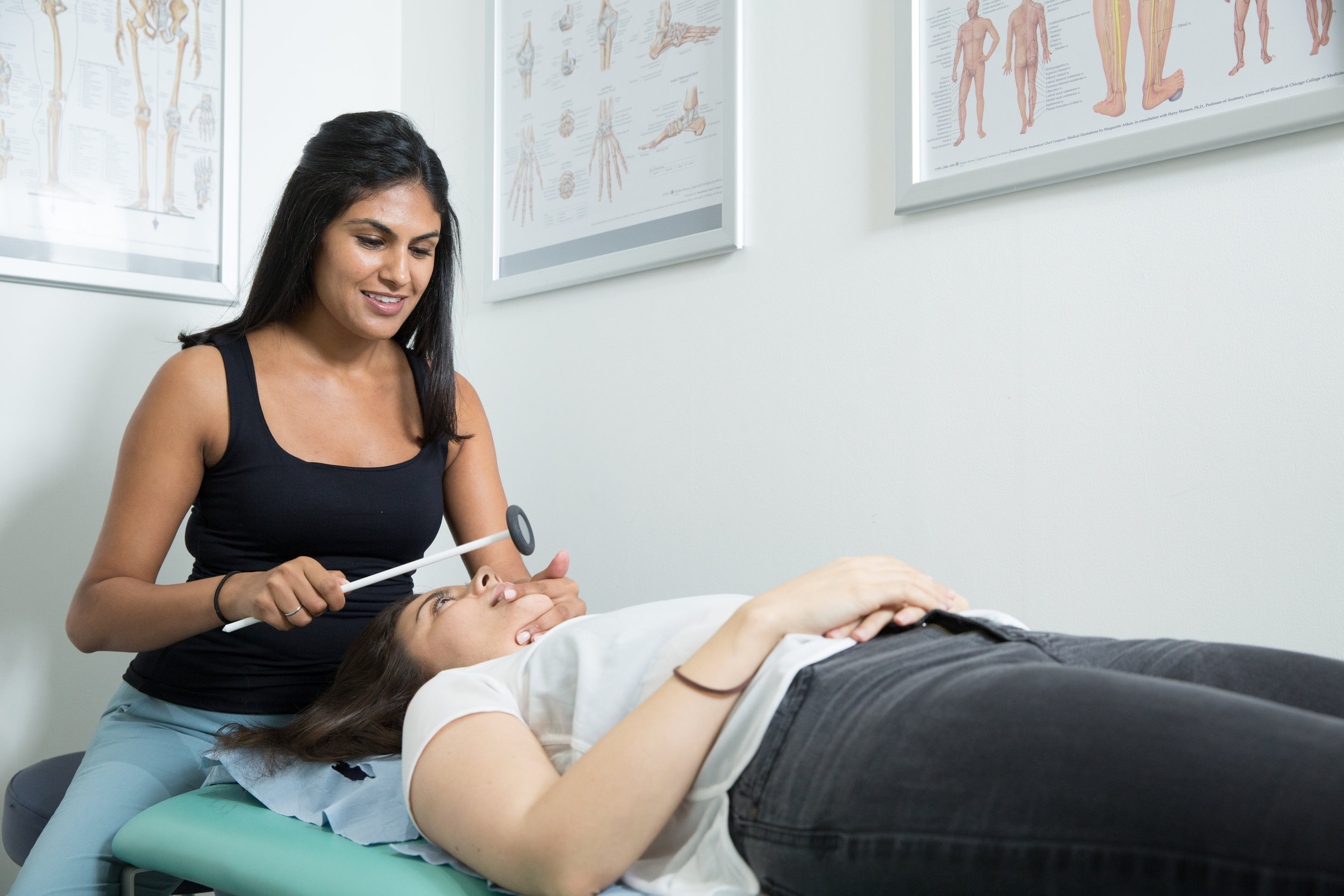
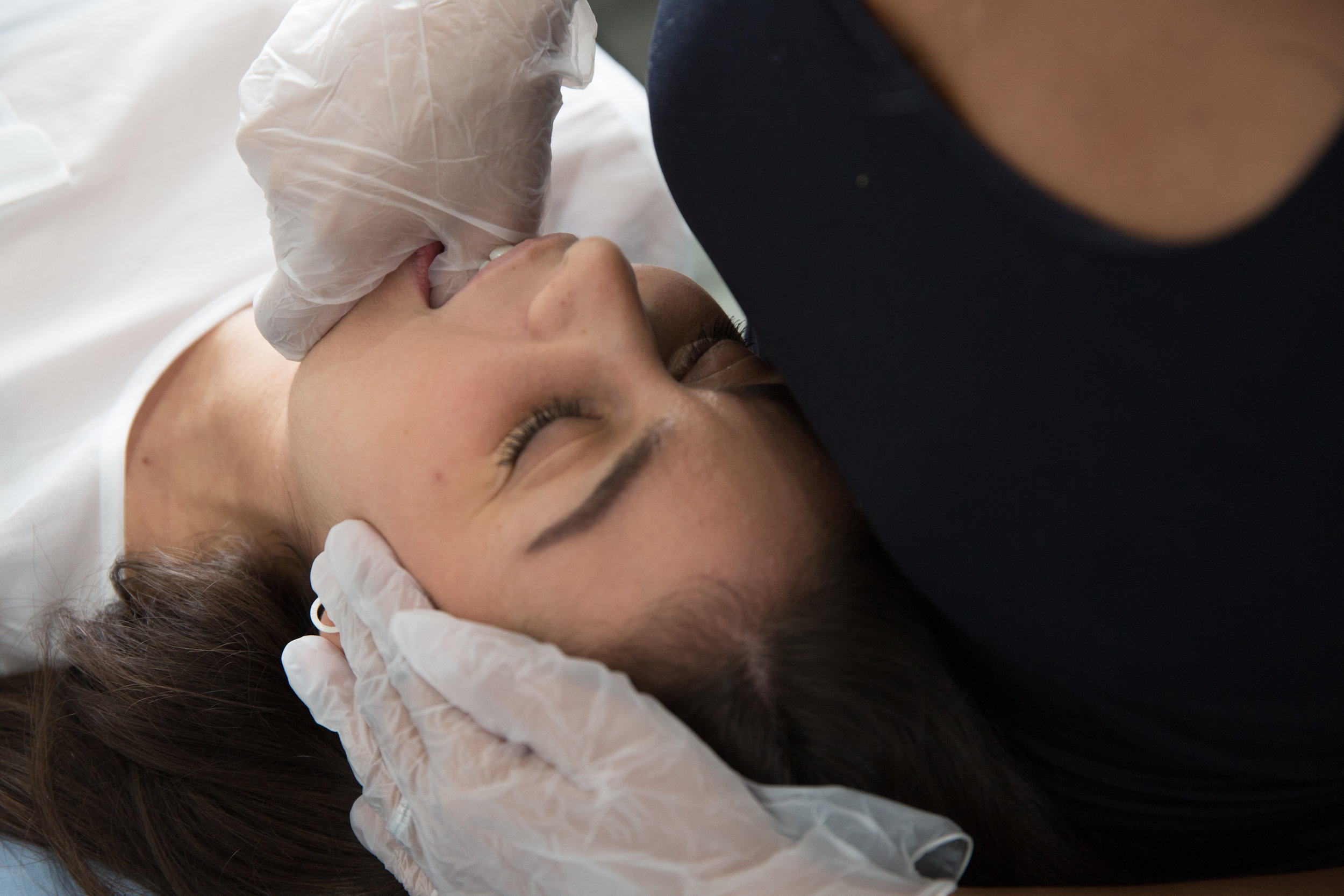
We can reduce your pain and restore range of movement with functional activities such as eating, talking and sleeping. Physiotherapy treatment varies from simple advice to extensive therapy. An initial assessment will see how your current problem is affecting your activities of daily living and a personalised treatment program will be designed which may include:
prescribing exercises to relieve pain and stiffness and improve muscle strength
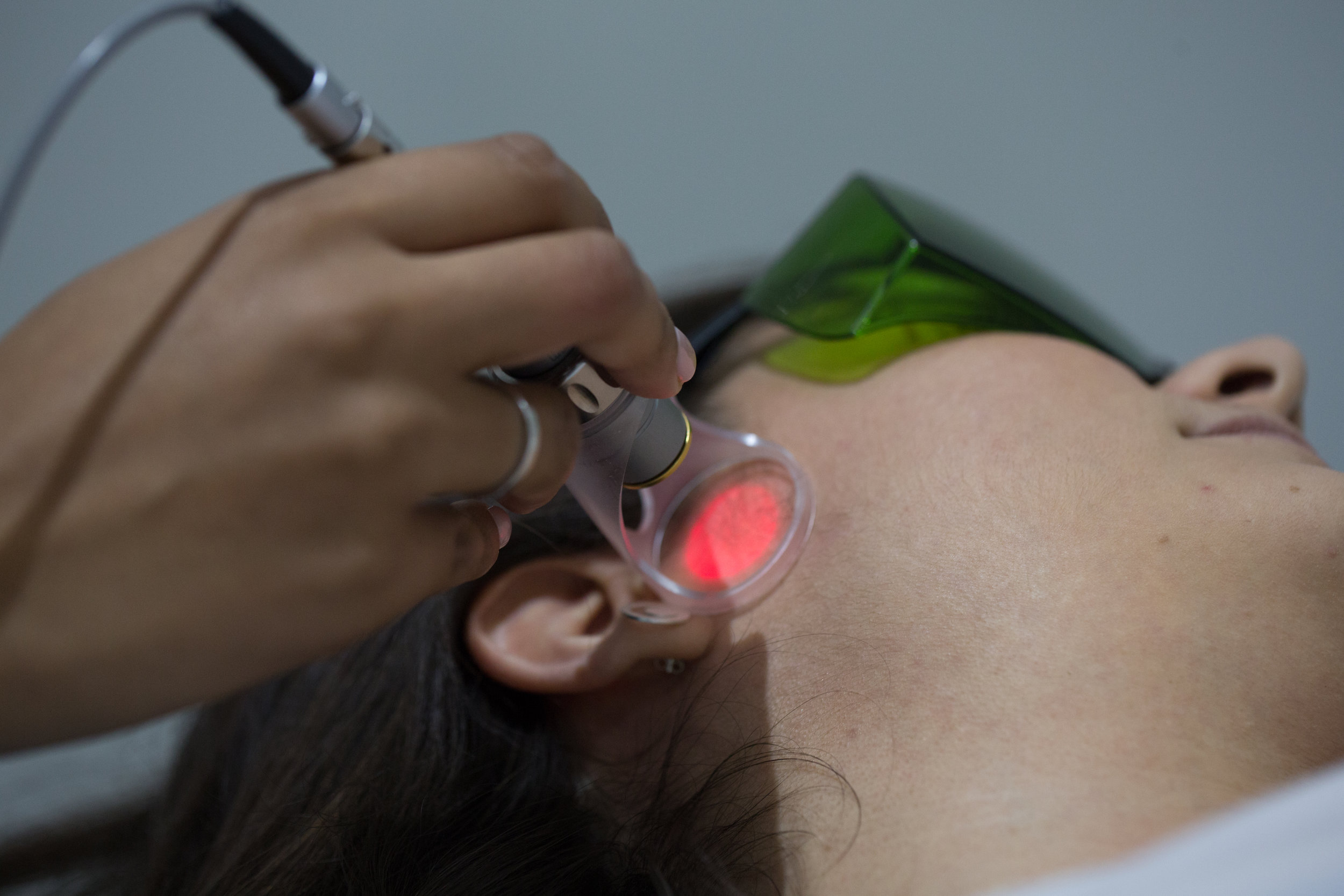
use electrotherapy modalities e.g. ultarsound, Low Level Laser Therapy, and heat/ice to promote healing and physical function
advice on ergonomic changes at work and at home
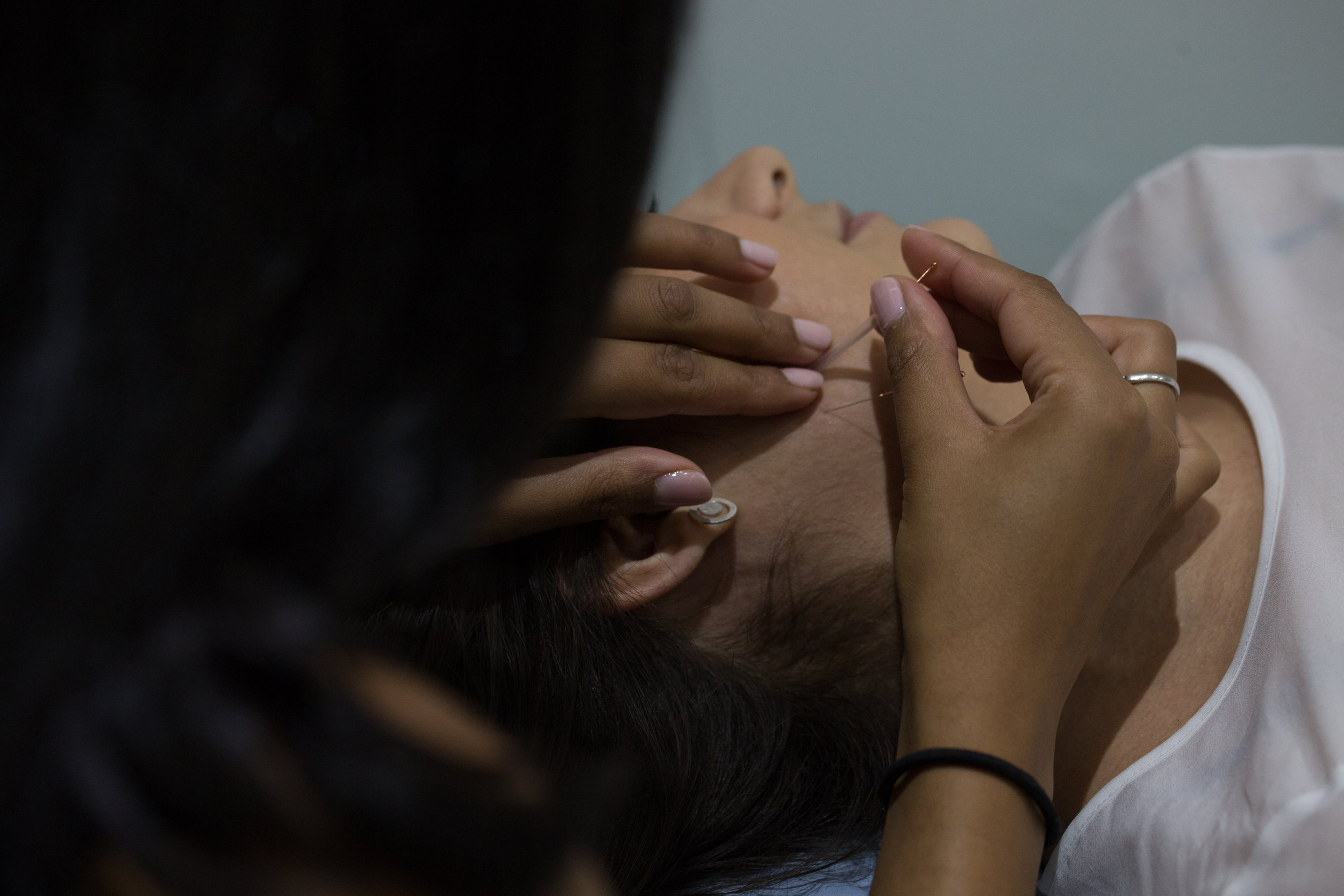
dry needling
mobilsations
stress management
lab testing
diagnostic scans
Experience and Colleagues I Work With
I have been fortunate to spend time with the likes of Steve Kraus DPT, Dr. Tannenbaum DDS, and with Dr. Jennifer Bassuir DDS and Meralee Guhl DPT at the Center for Oral, Facial and Head Pain at Columbia University in New York. Through all this experience I have been able to make an effective treatment plan. I also work very closely with Mr Piet Haers, Mr Kaveh Shakib, Mr Basil Mizrahi, Prof. Andrew Eder and Moira Wong as well as other Maxillofacial Surgeons and Dentists in and around London.